Can Antibiotics Cure Low Back Pain?
- At May 13, 2013
- By Healing In Motion
- In News
 0
0
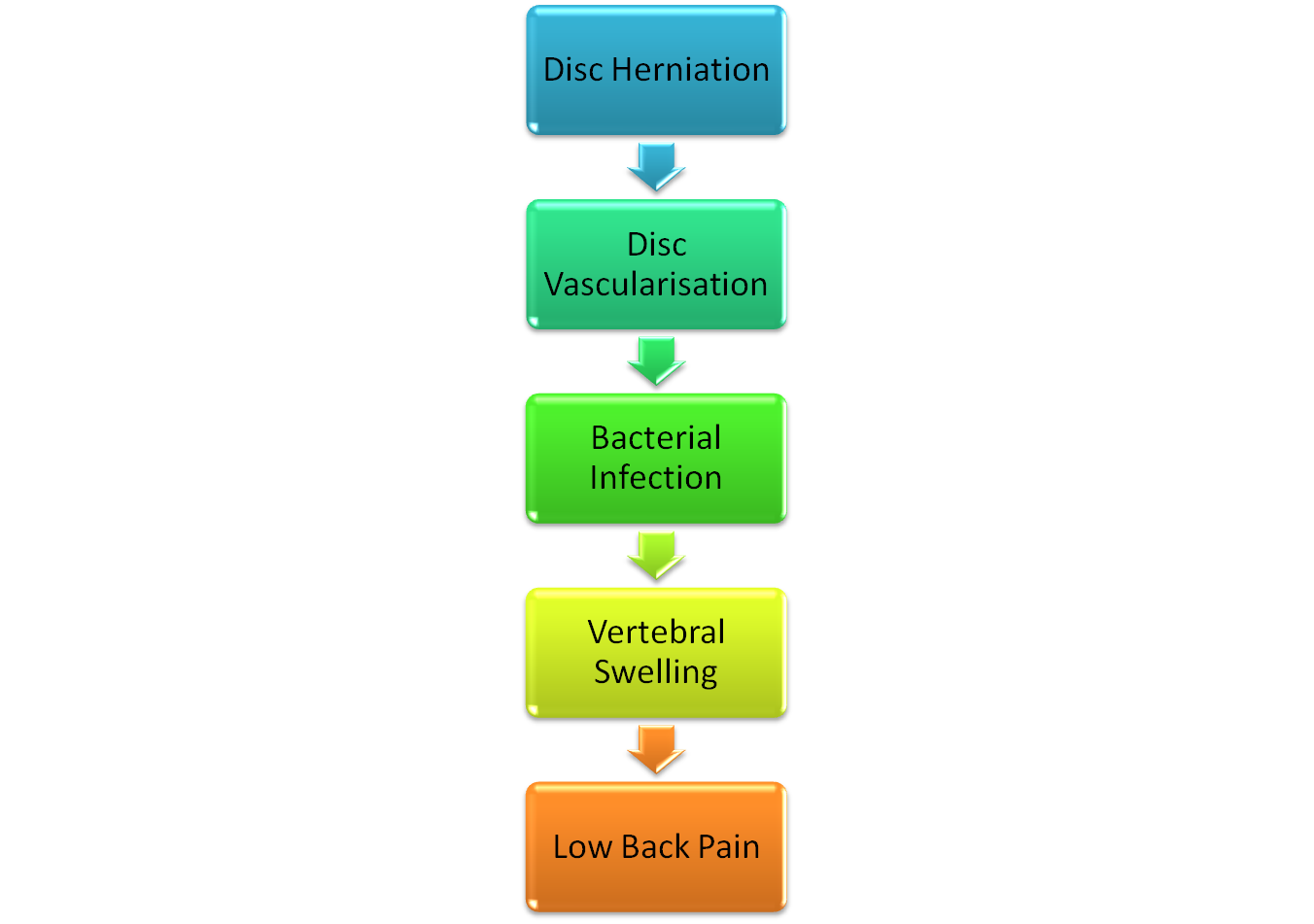
![]() Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
In their second study, Albert et al. conducted a double-blind randomised controlled trial with 162 patients whose only known illness was chronic low back pain of greater than 6 months duration occurring after a previous disc herniation. They also had bone edema in the vertebrae next to the previous herniation. The patients were split into 2 groups. One group was given antibiotics for 100 days and the other group was given a placebo for 100 days. The patients were evaluated at the start of treatment, at the end of treatment and 1 year after the end of treatment. The patients given antibiotics improved on all measures; they had less low back pain, less leg pain and better function and the changes were highly statistically significant.
Although these results are extremely encouraging, they should be confirmed with larger groups. Additionally, it’s worth bearing in mind that this form of treatment only applies to a subgroup of people with low back pain and that the indiscriminate use of antibiotics for low back pain should be discouraged as it could lead to decreased efficacy of antibiotics through the spread of drug-resistant bacteria.
Physiotherapy Is As Good As Surgery For Meniscal Tears
- At March 25, 2013
- By Healing In Motion
- In News
 0
0
Last week Yahoo! News reported that physiotherapy was as good as knee surgery. The claims were based on results of a recent study by Jeffrey Katz, Professor of Medicine and Orthopedic Surgery at Harvard University. The randomised controlled trial involved symptomatic patients aged 45 years or older with a meniscal tear and evidence of mild-to-moderate osteoarthritis on imaging. They randomly assigned 351 patients to surgery and postoperative physiotherapy or to a standardized physiotherapy regimen (with the option to cross over to surgery at the discretion of the patient and surgeon). The patients were evaluated at 6 and 12 months.
They did not find significant differences between the study groups in functional improvement 6 months after randomisation; however, 30% of the patients who were assigned to physiotherapy alone underwent surgery within 6 months. “Since both the patients who received physical therapy and those who received surgery had similar and considerable improvements in function and pain, our research shows … there is no single ‘best’ treatment. Patients who wish to avoid surgery can be reassured that physical therapy is a reasonable option, although they should recognize that not everyone will improve with physical therapy alone.” Katz said.
Having undergone a successful menisectomy last year I can personally attest that surgery can sometimes achieve results that physiotherapy can’t but conservative management such as physiotherapy should always be the first port of call.
Is Back Pain Genetic?
- At September 30, 2012
- By Healing In Motion
- In News
 0
0
There’s been a lot of talk in the press (BBC, The Telegraph, Yahoo, Medical News Today, etc.) this week about finding the gene that causes back pain. So now back pain can be added to a host of other inherited conditions such as obesity, depression, cancer and diabetes. Before I give my opinion, I’d like to specify exactly what recent research has found. The study was carried out at King’s College London and was published this month in the Annals of Rheumatic Diseases. They found an association between the PARK2 gene and lumbar disc degeneration (LDD). The PARK2 gene switches off in people with LDD. LDD is the progressive dehydration of lumbar discs leading to disc space narrowing and osteophyte (bony spurs) growth. It is thought to be a common cause of low back pain (LBP).
It’s interesting to note however, that only 5 % of the population is affected by LDD but over 80% of people will have an episode of LBP at some time in their lives. Also, lots of people diagnosed by MRI scan with LDD have not experienced low back pain…strange? The obvious conclusion is that most LBP is not caused by LDD. Now, let’s look more closely at the relationship between the PARK2 gene and LDD. Does having the PARK2 gene automatically lead to disc degeneration? No! The PARK2 gene has to be switched off for that to happen. What switches it off? That there is the million dollar question, and it hasn’t been answered to satisfaction. The researchers have alluded to environmental factors such as lifestyle and diet. This is starting to sound familiar…could this be the old ‘nature vs nurture’ debate again?
Epigenetics explains how genes can be switched on and off. It’s the study of mechanisms by which the environment controls gene activity. “These mechanisms can enable the effects of parents’ experiences to be passed down to subsequent generations eg. paternal grandsons of Swedish men who were exposed during preadolescence to famine in the 19th century were less likely to die of cardiovascular disease, if food was plentiful, then diabetes mortality in the grandchildren increased” (Wikipedia).
Being told that we have a gene for x, y or z disease can lead to a helpless condition where we believe we have no control over what happens to us and so we gloomily go down a predestined path. “I can’t do anything about it, it’s in my genes.” Incidentally, self-fulfilling prophecies can come into play here. On the other hand, epigenetics puts us firmly in the driver’s seat. We can control our environment by controlling what we do, how we think, what we eat, drink, etc. It empowers us to write our own scripts. Gattaca is a beautiful example of this…I know it’s only a film but wasn’t it good!
Coming back to LBP, nothing has changed. Acute back pain is often caused by physical factors such as poor lifting technique, twisting, and prolonged sitting. Whereas with chronic back pain, there is the added contribution of mental, emotional and social factors. The good news is that whether it is acute or chronic, there are lots of things that can be done to prevent, treat and manage low back pain.
Acupuncture NICE For Headaches
- At September 23, 2012
- By Healing In Motion
- In News
 0
0
The National Institute for Health and Clinical Excellence (NICE) has released its first clinical guideline on how to diagnose and manage headaches. It differentiates 4 types of headache: tension-type headaches, migraines, cluster headaches and medication overuse headaches. NICE recommends acupuncture as a treatment option for tension-type headaches and it says we should “consider a course of up to 10 sessions of acupuncture over 5–8 weeks for the prophylactic treatment of chronic tension-type headache”.
Pain And Perception
- At May 14, 2012
- By Healing In Motion
- In News
 0
0
I read an interesting article in BBC News Health a couple of weeks ago. It reviewed 2 recent studies on pain. The first was published in The Journal of Pain by Atsuo Yoshino et al. Subjects were shocked with an electric current whilst they were shown pictures of sad, happy or neutral faces. Photos of an emotional face usually provoke the same emotional response in the person viewing the picture. Although the electrical stimulation was the same in all cases, subjects felt more pain when looking at sad faces.
The second study was conducted by Marion Hofle et al. in Pain. The researchers asked the subjects to place one of their hands under a screen. On the screen, they played a video of a hand being pricked by a needle, poked by a cotton bud or just left alone. The subjects perceived the hand on the screen as their own. A painful or non-painful stimuli was applied simultaneously to the video. Viewing the needle prick increased the unpleasantness ratings of the stimulus.
As these studies have shown, negative emotional states and negative expectation seem to increase pain and so the mind plays an important role in the experience of pain. As a physiotherapist, dealing with pain is a daily occurrence and I can remember qualifying as an acupuncturist over 10 years ago…I was desperately keen to use my new skill on anyone that was willing to try and worked hard at convincing anyone that was hesitant to try! With those that were initially hesistant…possibly due to a slight needle aversion, I quickly noticed their exaggerated responses to acupuncture. I can remember several occasions when I would gently touch them with a finger or with the plastic guide tube that surrounds the needle and they would jump and shout “ouch”…to which I would reply “relax, we haven’t started yet!” I’ve now learnt from those experiences and no longer feel the need to convince everyone to have acupuncture…no matter how great I think it is!
John Milton was right in Paradise Lost…“The mind is its own place, and in itself can make a heaven of hell, a hell of heaven.”
An Integrated Approach To Low Back Pain Improves Results
- At April 26, 2012
- By Healing In Motion
- In News
 0
0
An article in Medical News Today reviews a study in The Journal of Alternative and Complementary Medicine on the treatment of low back pain. A combined program of complementary and conventional therapies was found to be more helpful than the usual care provided by the primary care physician. The benefits of the program were a decrease in pain and an improvement in function. The complementary therapies provided included physiotherapy, acupuncture, massage, mind-body techniques, chiropractic and nutritional advice. Healing in Motion in St Albans aims to treat musculoskeletal disorders using a holistic, integrated approach.
Metal On Metal Total Hip Replacements Unsafe?
- At March 5, 2012
- By Healing In Motion
- In News
 0
0
A BBC Newsnight and British Medical Journal investigation has prompted a lot of discussion regarding metal on metal total hip replacements. Lately, a study has found that the metal components rub against each other causing small particles to break away into surrounding tissues. This leads to elevated blood levels of metal ions such as cobalt and chromium. The clinical significance of this is still unknown. The Medicines and Healthcare products Regulatory Agency (MHRA) have stated that annual blood tests should be conducted to check levels of cobalt and chromium. If levels are high, an MRI scan should be carried out to see if the prosthesis requires revision.
A recent technology overview conducted by the American Academy of Orthopaedic Surgeons (AAOS) has concluded that metal on metal implants are at greater risk of revision than replacements with different bearing surface combinations. This has come as a bit of a surprise as it was hoped that sturdy metal on metal implants would outlast metal on plastic implants. It was also noted that larger femoral head components are at higher risk than smaller ones and older patients also incur a greater likelihood of requiring another operation.
A previous technology review had found that hip resurfacing is more likely to need revising than total hip arthroplasties (THA). The size of the head is inversely related to the risk of revision. However, the Australian registry has suggested that younger men have less risk of revision with resurfacing than they do with THAs. This is interesting because research published in this month’s The Journal of Bone & Joint Surgery (British Volume) shows that the 10 year survival rate for a Birmingham hip resurfacing (BHR) is 89.1% for women and 97.5% for men. Mr AJ Shimmin et al. conclude that “BHR provides good functional outcome and durability for men, at a mean follow-up of ten years. We are now reluctant to undertake hip resurfacing in women with this implant”.
All this definitely provides food for thought and it’s well worth doing some research and having a long chat with your surgeon before deciding what sort of hip prosthesis to have.
Acupuncture Awareness Week
- At February 26, 2012
- By Healing In Motion
- In News
 0
0
This week the British Acupuncture Council is launching the very first Acupuncture Awareness Week and their website is full of useful information. Of all the treatments I use, acupuncture is by far the one that most clients are curious about. Acupuncture has been used in China for over 2000 years. Fine needles are inserted into the skin to stimulate the body. Obviously, the needles are sterile and disposed of after use. Acupuncture can help with all sorts of muscle or joint pains like back pain for instance. The most common question is; how does it work? Let’s use back pain as an example (the following information was provided by the British Acupuncture Council).
“Acupuncture can help back pain by:
- Providing pain relief – by stimulating nerves located in muscles and other tissues, acupuncture leads to release of endorphins and other neurohumoral factors and changes the processing of pain in the brain and spinal cord (Pomeranz 1987; Zhao 2008).
- Reducing inflammation – by promoting release of vascular and immunomodulatory factors (Kim 2008, Kavoussi 2007;Zijlstra 2003).
- Improving muscle stiffness and joint mobility – by increasing local microcirculation (Komori 2009), which aids dispersal of swelling and bruising.
- Reducing the use of medication for back complaints (Thomas 2006).
- Providing a more cost-effective treatment over a longer period of time (Radcliffe 2006;Witt 2006).
- Improving the outcome when added to conventional treatments such as rehabilitation exercises (Ammendolia 2008; Yuan 2008).”
- Releasing tight bands in muscles
Following research into the effects of acupuncture on low back pain, the National Institute for Health and Clinical Excellence (NICE) now recommend that GPs offer a course of 10 sessions of acupuncture as a first line treatment for persistent, non-specific low back pain.
Hypermobile Sportsmen Are More Injury Prone
- At January 26, 2012
- By Healing In Motion
- In News
 0
0
Hypermobility can simply be described as joints bending and stretching further than normal. For instance, knees or elbows that bend backwards, a little finger that can bend backwards past 90 degrees, a thumb that can be bent to touch the forearm, etc.
An article in Reuters has summarised research that proves that hypermobile sportsmen are more prone to injury. Not only are they more likely to get injured but the injuries they sustain tend to be more serious. This could be due to a mix of factors such as weaker ligaments and soft tissue, and to poor joint positioning.
The likelihood of injury could be remedied by working on joint positional awareness and by muscle strengthening and coordination exercises to support the joints.
Acupuncture Helps Reduce Stress
- At December 22, 2011
- By Healing In Motion
- In News
 0
0
An article in today’s Mail Online reviews research carried out on the effects of acupuncture on stressed rats. The results show that acupuncture can reduce the levels of a protein linked to stress. Apparently this is the first study to show molecular proof of the benefit of acupuncture on stress.