Pain and Sleep
- At February 4, 2019
- By Healing In Motion
- In Research
 0
0
![]()
A few days ago, Krause et al. from the University of California (Berkeley), published the results of their research on the relationship between pain and sleep. They found that poor sleep quality was linked to increases in pain experience, whereas better sleep quality decreased pain. Krause notes that “the results clearly show that even very subtle changes in nightly sleep – reductions that many of us think little of in terms of consequences – have a clear impact on your next-day pain burden”. In the laboratory, they were able to identify that sleep deprivation amplifies the reactivity in parts of the brain (somatosensory cortex) responsible for the perception of pain. Whilst deactivating the responses from some pain relieving centres (insula and nucleus accumbens).
The irony is that pain often disrupts sleep, and thus the pain experience gets magnified and a vicious cycle is created.
Acceptance and Commitment Therapy Helpful for Chronic Pain
- At July 22, 2017
- By Healing In Motion
- In Research
 0
0
![]()
Yu et al recently published the results their study on the effects of acceptance and commitment therapy (ACT) in people with chronic pain. The article appeared in last month’s issue of Journal of Pain. ACT “is an empirically-based psychological intervention that uses acceptance and mindfulness strategies mixed in different ways with commitment and behavior-change strategies, to increase psychological flexibility. The objective of ACT is not elimination of difficult feelings; rather, it is to be present with what life brings us and to “move toward valued behavior”. Acceptance and commitment therapy invites people to open up to unpleasant feelings, and learn not to overreact to them, and not avoiding situations where they are invoked” (Wikipedia).
The study involved over 400 hundred adults referred to a pain management clinic. Treatment significantly improved pain acceptance, pain-related interference, work and social adjustment and depression. This was true immediately post-treatment as well as at a 9-month follow-up. ACT also changed something known as “self-as-context” (SAC). SAC can be described as “the you that is always there observing and experiencing and yet distinct from one’s thoughts, feelings, sensations, and memories” (Wikipedia). Of note was the fact that positive changes in “self-as-context” were associated with positive changes in outcomes.
It’s really interesting how acceptance and commitment therapy has incorporated Buddhist principles and techniques such as mindfulness, acceptance and the self. In fact, it seems that the use of Buddhist philosophy and principles are becoming more common within therapy nowadays.
Chronic Pain Linked to Memory Decline and Dementia
- At June 14, 2017
- By Healing In Motion
- In Research
 0
0
![]()
A study by Whitlock et al from the University of California, published in this month’s Jama Internal Medicine, looked into the relationship between persistent pain, memory decline and dementia. Over 10,000 senior citizens (median age of 73 years) from the Health and Retirement Study were followed for 12 years.
At baseline, persistent pain affected 11% of participants and was linked with more restrictions in daily activities and more symptoms of depression. Those with persistent pain had a greater risk (9%) of having a more rapid memory decline than those without pain. They also had a smaller increase in risk (2%) of developing dementia. These changes significantly increased the chances of being unable to manage medications (16%) or finances (12%).
What’s the causal connection between chronic pain, memory decline and dementia? The authors believe the severity of pain can decrease attention capacity and impair memory consolidation. Additionally, pain leads to stress, and stress has been shown to promote cognitive decline, mainly through hypotrophy of the hippocampus. In my opinion, the disruption of sleep can also contribute to poor memory and a decline in cognitive ability because, as we know, sleep is involved in memory processing and consolidation.
Fortunately, physiotherapy, rehabilitation, relaxation and mindfulness meditation are effective at addressing chronic pain.
Shared Reading Improves Mood and Decreases Pain
- At April 12, 2017
- By Healing In Motion
- In Research
 0
0
google-site-verification: googleec220f26f2a6a6de.html![]()
Earlier this year Billington et al. from the University of Liverpool published the results of their study looking at the effects of shared reading (SR) on people with chronic pain. The shared reading model they used was the one employed by the charity “The Reader“. “The Reader is an award-winning charitable social enterprise working to connect people with great literature through shared reading. We’re here to bring books to life, creating welcoming environments in which personal feeling is recognised and valued, forming vital connections between people and literature through which everyone can feel more alive.”
The researchers concluded “Qualitative evidence indicates SR’s potential as an alternative or long-term follow-up or adjunct to CBT in bringing into conscious awareness areas of emotional pain otherwise passively suffered by patients with chronic pain. In addition, quantitative analysis, albeit of limited pilot data, indicated possible improvements in mood/pain for up to 2?days following SR. Both findings lay the basis for future research involving a larger sample size.”
The preliminary findings are encouraging. There may be other factors such as distraction, social bonding and the benefits of having regular scheduled activities that may also play a part in improving the well-being of the participants.
Persistent Pain Associated With DNA Changes In Brain And Immune Systems
- At February 1, 2016
- By Healing In Motion
- In Research
 0
0
![]()
Renaud Massart et al from McGill University have recently published an article in Scientific Reports on the effects of chronic pain on the body. “Chronic pain” is pain that has lasted for 6 months or more. The study was performed on rats with induced nerve injuries.
The results showed epigenetic changes in the DNA of the prefrontal cortex and in the DNA of T cells. Their findings support the notion that persistent pain affects multiple biological systems. It’s possible that future research will show changes to other systems as well.
New Pain Mechanisms Revealed
- At March 30, 2015
- By Healing In Motion
- In Research
 0
0
Neuropathic pain is a chronic pain condition caused by a damaged or dysfunctional nervous system. It is characterised by shooting and burning pain that lasts long after the initial onset. Common causes of neuropathic pain include:
- alcoholism
- amputation
- back, leg and hip problems
- chemotherapy
- diabetes
- facial nerve problems
- HIV or AIDS
- multiple sclerosis
- shingles
- spine surgery
Unfortunately neuropathic pain doesn’t respond much to conventional analgesics but instead, antidepressants (amitriptyline and duloxetine) and anticonvulsants (gabapentin and pregabalin) have been found to help relieve pain.
A new study published in this month’s edition of Neuron by Thomas Nevian et al from the Department of Physiology at the University of Bern has revealed some of the mechanisms involved in neuropathic pain. In a mouse model, they found that neurons in the gyrus cinguli, a part of the brain found in the limbic system (usually associated with emotion) are modified by pain forming a “pain memory”. Neurons in the gyrus cinguli become more excitable due to a down-regulated ion channel. This leads to an increased number of nerve impulses which the brain perceives as pain.
The researchers managed to restore the function of the ion channel by activating a receptor sensitive to serotonin. This explains the success of some antidepressants in treating neuropathic pain. Nevian et al were able to identify the specific subtype of serotonin receptor that was more efficient at reducing the perception of pain. Excitingly, this could lead to the development of more effective drugs to treat neuropathic pain.
Meditation Decreases Chronic Neck Pain
- At March 23, 2015
- By Healing In Motion
- In Research
 0
0
A group of German researchers recently published the results of a study looking into the benefits of meditation on people with chronic neck pain. The article was published in The Journal of Pain. They studied about 90 people who had neck pain for an average of 11 years. The average age of the participants was 50 years. Their results found significant improvements in pain reduction and pain coping but no effect on functional disability.
The findings suggest that meditation could be used as an adjunct alongside physical treatments that provide functional benefits.
Vitamin D Deficiency Linked To Chronic Pain
- At May 18, 2014
- By Healing In Motion
- In Research
 0
0
Paul McCabe et al from the University of Manchester analysed data from the European Male Ageing Study and found that men with vitamin D deficiency at the start of the study were more than twice as likely to experience ongoing widespread pain over the next 4 years as those with high levels of vitamin D. It was noted that the men with chronic widespread pain were more likely to be physically active, obese, depressed and to have other health problems. Once these other factors were taken into account the link between vitamin D and pain disappeared.
However, John McBeth et al analysed data from the same study and found that even after adjusting for other health factors, pain remained moderately associated with increased odds of having low vitamin D levels. This is supported by a 5-year longitudinal study published last year by Laura Laslett et al in which vitamin D deficiency was found to predict incidence or worsening of knee pain and hip pain.
There seems to be a link between a deficiency of vitamin D and pain but could supplementation with vitamin D help to decrease pain? Between 2008 and 2010, Shreuder et al conducted a study in Holland and they did indeed find a small positive benefit (less pain and better function) after taking a high dose of vitamin D for 6 weeks.
What could the mechanism behind vitamin D and pain be? Tague et al found that vitamin D deficiency in rats can lead to a hyperinnervation of skeletal muscle which is likely to contribute to muscle hypersensitivity and pain.
Vitamin D is naturally present in a few dietary sources such as fish oils, mushrooms, eggs and liver. Other than supplements, sunlight exposure is the best source of vitamin D for most of people.
Potential Advances In The Treatment Of Osteoarthritic Pain
- At March 2, 2014
- By Healing In Motion
- In Research
 0
0
In a recent study published in Annals of the Rheumatic Diseases and reported in Medical News Today, Sara Kelly and colleagues from the Arthritis Research UK Pain Centre at The University of Nottingham have discovered a new way to possibly decrease the chronic pain affecting people with osteoarthritis. They studied a protein receptor called TRPV1 which is present in the synovial membranes of joints. These receptors are responsive to pain. Injecting TRPV1 agonists directly into the joint produced pain relieving effects.
The study was performed on rats so before being used on humans the results will need to be replicated in clinical trials and monitored for potential side effects.
Until then the best self-help advice for those with osteoarthritis is weight loss (if it affects joints in the lower limbs), stretching & strengthening exercises and maintaining moderate levels of activity. Nutritional supplements can also help (see related articles here).
Can Antibiotics Cure Low Back Pain?
- At May 13, 2013
- By Healing In Motion
- In News
 0
0
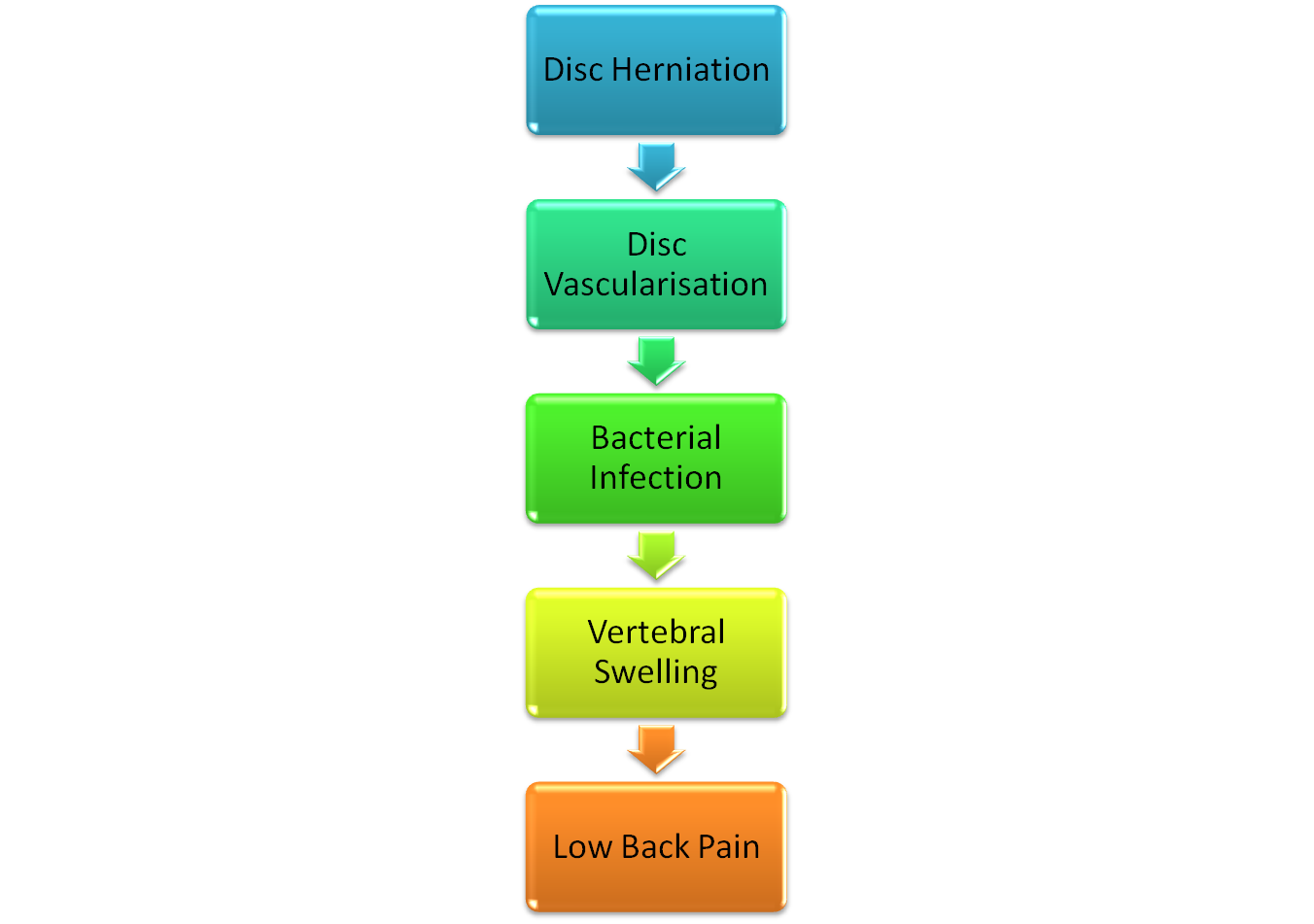
![]() Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
In their second study, Albert et al. conducted a double-blind randomised controlled trial with 162 patients whose only known illness was chronic low back pain of greater than 6 months duration occurring after a previous disc herniation. They also had bone edema in the vertebrae next to the previous herniation. The patients were split into 2 groups. One group was given antibiotics for 100 days and the other group was given a placebo for 100 days. The patients were evaluated at the start of treatment, at the end of treatment and 1 year after the end of treatment. The patients given antibiotics improved on all measures; they had less low back pain, less leg pain and better function and the changes were highly statistically significant.
Although these results are extremely encouraging, they should be confirmed with larger groups. Additionally, it’s worth bearing in mind that this form of treatment only applies to a subgroup of people with low back pain and that the indiscriminate use of antibiotics for low back pain should be discouraged as it could lead to decreased efficacy of antibiotics through the spread of drug-resistant bacteria.