Manage Longstanding Low Back Pain by Spending Time in Nature
- At June 26, 2025
- By Healing In Motion
- In Research
 0
0
Study Overview
The article “Being away from everything”: Exploring the importance of access to nature for individuals living with chronic low back pain, published in the Journal of Pain, investigates how nature can aid in managing chronic low back pain (cLBP). It involved ten semi-structured interviews with people averaging 50.1 years old and living with cLBP for about 19.1 years.
Key Findings
The study found that nature can provide distraction, reduce isolation, and offer a calming environment, enhancing pain self-management. However, many face challenges like physical disabilities, environmental hazards, or lack of proximity to natural spaces. It suggests integrating nature-based activities into treatment plans and exploring virtual reality for those unable to access nature.
Detailed Analysis and Background
The article presents a pioneering qualitative cross-sectional study focused on understanding the role of natural environments in managing chronic low back pain (cLBP). The study, conducted and published in June 2025, addresses the growing evidence against the effectiveness of ‘one-size-fits-all’ pharmacological approaches, advocating for alternative non-pharmacological therapies such as green social prescribing and spending time in nature.
Methodology and Participants
The research methodology involved ten semi-structured interviews, primarily with women (9 out of 10 participants), with an average age of 50.1 years and an average duration of living with cLBP of 19.1 years. This qualitative approach aimed to explore the lived experiences of individuals, providing deep insights into their coping strategies and the role of nature in ameliorating pain. The analysis was conducted using Reflexive Thematic Analysis, identifying two main themes: (1) Importance of Nature and (2) Inaccessible Nature, each with four subthemes respectively.
Key Findings and Themes
The theme “Importance of Nature” underscores the benefits of accessing natural environments, which can significantly aid in self-management of cLBP. Participants reported that being in nature offered distraction, reduced feelings of isolation, and provided a calming environment, which helped alleviate pain and improve mental well-being. For instance, those able to immerse themselves in larger green spaces, such as forests, felt more positive, as they could lose themselves in the environment and focus less on their pain levels.
However, the theme “Inaccessible Nature” revealed significant barriers, including physical disabilities, environmental obstacles or hazards, and geographical limitations. These challenges often undermined the ability to access nature, highlighting an unmet clinical need. The study emphasizes that many individuals encounter substantial obstacles, such as uneven terrain, limited seating, or difficulties leaving their homes, making it challenging to benefit from the restorative properties of nature.
Implications and Recommendations
The findings suggest that integrating nature-based activities into treatment plans could be beneficial, offering a promising avenue for improving overall well-being for those with cLBP. The researchers recommend exploring virtual reality interventions to simulate nature experiences for those unable to access outdoor spaces, addressing accessibility issues. This approach could help make the benefits of nature accessible to everyone, potentially through technological innovations. Simple changes, such as better paths and seating, were also suggested to enhance real-world access.
The study marks the first qualitative investigation focusing directly on the nuanced role of natural settings within the coping mechanisms employed by people with cLBP. This pioneering aspect underscores the need for further research into how nature can be incorporated into holistic and multidisciplinary frameworks for treating pain, aligning with leading international organizations’ recommendations.
Contextual Background
Chronic low back pain is a major public health issue, with the highest prevalence globally among musculoskeletal conditions and being the leading cause of disability worldwide. It affects individuals of all ages, with peak cases at 50–55 years, and women experiencing it more frequently. The condition often leads to work loss, participation restriction, and reduced quality of life, making innovative approaches like nature-based interventions particularly relevant.
The study’s emphasis on accessibility challenges also aligns with broader discussions on health equity, addressing significant physical barriers faced by people living with chronic pain, as highlighted in the University of Plymouth news release. This includes the need for better infrastructure, such as improved paths and seating, to facilitate access to natural spaces.
Conclusion
In conclusion, the article provides valuable insights into the therapeutic potential of nature for individuals with cLBP, while also highlighting significant accessibility barriers. It advocates for innovative solutions like virtual reality to bridge these gaps, contributing to the broader discourse on holistic pain management. The findings are particularly timely, given the current understanding of cLBP as a major global health challenge, and offer a foundation for future research into nature-based interventions.
Chronic Low Back Pain, Bacterial Infection, and Antibiotic Treatment
- At April 21, 2025
- By Healing In Motion
- In Research
 0
0
Chronic low back pain (CLBP) is a leading cause of disability globally, affecting millions and posing significant challenges to healthcare systems due to its complex aetiology and limited effective treatments (Gilligan et al., 2021). Recent research has sparked debate by suggesting that low-grade bacterial infections, particularly involving Cutibacterium acnes (C. acnes), may contribute to CLBP in a subset of patients, especially those with disc herniation and Modic Type 1 changes (bone oedema visible on MRI). This hypothesis, if validated, could revolutionise treatment by introducing antibiotics as an alternative to conventional therapies or invasive procedures like spinal surgery. However, the evidence remains controversial, with concerns about contamination, antibiotic efficacy, and stewardship. The following summary synthesises findings from key studies, highlighting microbiology evidence, clinical trial outcomes, and ongoing research challenges.
Microbiology Evidence: Bacterial Presence in Herniated Discs
Several studies have investigated whether bacteria, particularly C. acnes, are present in herniated disc tissue and contribute to CLBP. Gilligan et al. (2021) reviewed five well-designed microbiology studies that confirmed bacteria in disc samples, suggesting infection rather than contamination. These studies found C. acnes, a low-virulence anaerobic bacterium commonly associated with acne, in herniated disc tissue, particularly in patients with Modic Type 1 changes. However, the bacterial burden was low, potentially below detection limits in some studies, which may explain conflicting results where bacteria were absent or attributed to surgical contamination (Gilligan et al., 2021).
Astur et al. (2023) conducted a prospective cohort study to identify bacteria in herniated intervertebral discs, reporting C. acnes in a significant proportion of samples. Their stringent aseptic protocols minimised contamination risks, supporting the infection hypothesis. Similarly, Urquhart et al. (2015) conducted a systematic review and found moderate evidence that low-virulence bacteria are present in spinal disc material, particularly in patients with disc herniation and Modic Type 1 changes. They applied Bradford Hill’s criteria to assess causation, concluding modest evidence for a causal link but noting the need for further research to distinguish infection from contamination (Urquhart et al., 2015).
In contrast, Monge-García et al. (2024) explored whether bacterial presence in disc cultures represents true infection or contamination. Their study suggested that while C. acnes was frequently detected, contamination during surgical procedures could not be ruled out, particularly given the bacterium’s ubiquity on skin and in hair follicles. This raises a critical question: are bacteria in disc tissue causative agents of CLBP or incidental findings due to procedural artefacts? The conflicting findings underscore the need for standardised microbiological methods and larger sample sizes to clarify the role of C. acnes (Monge-García et al., 2024).
Clinical Evidence: Antibiotic Efficacy in CLBP
Clinical trials have tested whether antibiotics can reduce pain and disability in CLBP patients with suspected bacterial infections. Two randomised controlled trials (RCTs) reviewed by Gilligan et al. (2021) demonstrated significant pain and disability reductions in patients with CLBP and Modic Type 1 changes treated with oral antibiotics, typically amoxicillin-clavulanate, for up to 100 days. These patients, often unresponsive to conventional treatments like physiotherapy or analgesics, showed clinically meaningful improvements, suggesting antibiotics as a potential alternative to surgery for those facing disc replacement or fusion (Gilligan et al., 2021).
A landmark RCT by Albert et al. (2013), cited across multiple articles, found that 100 days of amoxicillin-clavulanate significantly reduced pain and disability in patients with CLBP post-disc herniation and Modic Type 1 changes compared to placebo. At one-year follow-up, the antibiotic group reported a median Roland Morris Disability Questionnaire (RMDQ) score reduction from 15 to 7, compared to 15 to 14 in the placebo group (p=0.0001). Pain scores and constant pain prevalence also improved significantly (Urquhart et al., 2015; Gilligan et al., 2021). However, the trial reported high rates of adverse events, particularly gastrointestinal issues like diarrhoea, in 65% of the antibiotic group versus 23% in the placebo group, raising concerns about tolerability (Urquhart et al., 2015).
Despite these promising results, not all studies support antibiotic efficacy. Some trials reported modest or non-significant effects, potentially due to underdosing or variable bacterial susceptibility. A review by Czaplewski et al. (2023) highlighted that oral amoxicillin doses (500–1000 mg, two or three times daily) may not achieve adequate intradiscal concentrations to target C. acnes effectively, with only 6.5% of serum concentrations reaching herniated disc tissue. Higher doses (e.g., 1000 mg three times daily) may be needed to reach efficacy targets for 90% of C. acnes strains, suggesting that previous studies may have been underdosed (Czaplewski et al., 2023).
Modic Changes and Infection Hypothesis
Modic Type 1 changes, characterised by vertebral bone oedema, are six times more prevalent in CLBP patients than the general population and are strongly associated with the infection hypothesis. Aebi (2013) noted that 80% of discs infected with C. acnes in surgical samples developed Modic Type 1 changes, suggesting that bacterial infection may trigger inflammation and oedema in adjacent vertebrae (Aebi, 2013). The neovascularisation following disc herniation is thought to allow C. acnes to enter the disc during transient bacteraemia, such as during tooth brushing, leading to chronic low-grade infection (Urquhart et al., 2015).
However, Modic changes may also result from mechanical stress or degeneration, complicating the attribution to infection alone. Lings (2013) and Rolfsen et al. (2024) emphasised that Modic Type 1 and Type 2 changes might represent different stages of a common degenerative process, questioning the specificity of infection as a cause. Rolfsen et al. (2024) proposed a multicentre case-control biopsy study to further investigate bacterial growth in CLBP patients with Modic changes, aiming to use advanced microbiological techniques like PCR to detect low-burden infections and control for contamination (Rolfsen et al., 2024).
Controversies and Challenges
The hypothesis that bacterial infection causes CLBP faces several challenges. First, the presence of C. acnes in disc tissue may reflect contamination rather than infection, given its prevalence on skin and difficulty in culturing due to its anaerobic nature (Monge-García et al., 2024). Second, the clinical significance of antibiotic benefits is debated, with some studies showing only modest effects and high adverse event rates (Gilligan et al., 2021). Third, long-term antibiotic use raises concerns about antimicrobial resistance and secondary infections like Clostridium difficile (Urquhart et al., 2015).
Antibiotic stewardship is a critical issue. The prolonged regimens (up to 100 days) used in trials contrast with typical short-course antibiotic treatments, increasing risks of resistance and side effects. Aebi (2013) and Lings (2013) cautioned against widespread antibiotic use without robust evidence, drawing parallels with the paradigm shift in peptic ulcer treatment following Helicobacter pylori discovery but urging caution until confirmatory studies are conducted.
Future Directions
The reviewed studies advocate for further research to refine patient selection, optimise antibiotic regimens, and address stewardship concerns. Rolfsen et al. (2024) and Czaplewski et al. (2023) emphasised the need for studies incorporating advanced diagnostics (e.g., quantitative microbiology, proteomics) and pharmacokinetic/pharmacodynamic evaluations to ensure adequate intradiscal antibiotic concentrations. Identifying biomarkers, such as cytokine patterns or genetic predispositions, could help select patients most likely to benefit from antibiotics (Gilligan et al., 2021).
Moreover, alternative delivery methods, such as intradiscal antibiotic injections (e.g., PP353, a novel treatment combining linezolid and a thermosensitive gel), are being explored to minimise systemic side effects and improve efficacy (Tripathi et al., 2025, cited in The Guardian). These approaches could offer targeted treatment for infection-related CLBP, reducing the need for prolonged oral antibiotics.
Conclusion
The hypothesis that low-grade bacterial infections contribute to CLBP, particularly in patients with disc herniation and Modic Type 1 changes, is supported by microbiological evidence and some clinical trials demonstrating antibiotic efficacy. However, controversies persist regarding contamination, variable clinical outcomes, and antibiotic stewardship. While antibiotics offer a potential alternative to surgery for a subset of CLBP patients, widespread adoption requires further validation through rigorous, multicentre studies. Future research should focus on optimising diagnostics, treatment regimens, and patient selection to balance efficacy with safety, potentially transforming the management of this debilitating condition.
Antibiotics For Low Back Pain?
- At March 31, 2025
- By Healing In Motion
- In Research
 0
0
Persica Pharmaceuticals has developed PP353, an intradiscal injection designed to treat chronic low back pain linked to bacterial infections, particularly cases associated with Modic changes (pathological alterations in vertebrae seen on MRI). PP353 combines:
- Linezolid (antibiotic) – targets bacterial infection
- Iohexol (contrast agent) – aids imaging and distribution
- Thermosensitive gel – ensures controlled release
Recent Study & Findings
- Conducted on 44 patients
- Patients received two injections four days apart
- 60% reported significant pain and disability reduction
- Study supports infectious origins in some chronic back pain cases
Potential Impact
- Could benefit the 25% of chronic low back pain cases linked to bacterial infection
- Offers a minimally invasive alternative to surgery or long-term medication
- Further clinical trials required before widespread use
Low Back Pain Could Affect How We Eat
- At February 28, 2022
- By Healing In Motion
- In Research
 0
0
A recent study by Lin et al. uncovered a relationship between longstanding low back pain and a preference for fat-rich foods. The authors found that the nucleus accumbens may be linked to the change in eating behaviour. The nucleus accumbens is a part of the brain that plays an important role in reward and pleasure processing. This could partly explain the high prevalence of obesity in people with longstanding pain.

Atherosclerosis and Low Back Pain
- At May 27, 2019
- By Healing In Motion
- In Research
 0
0
![]()
Atherosclerosis is well-known for its role in the development of coronary heart disease and stroke. The vascular occlusion that it causes leads to the infarction of heart and brain tissue. But coronary and cerebral blood vessels are by no means the only vessels that become clogged by atheromatous plaques. In 1993, Kauppila et al., from the department of forensic medicine at Helsinki University, postulated that insufficient arterial blood flow may play a role in low back pain. Their post-mortem angiographic study found that, compared to controls, significantly more people with a history of low back pain had anomalies in the arteries that supplied the lumbar spine – the arteries were narrowed by atheromatous lesions and some were completely missing.
Since that landmark study, several cadaver and clinical studies have corroborated the link between stenosis (and occlusion) of the lumbar arteries and the presence of low back pain. In fact, many studies have found an association between the aforementioned lumbar vascular insufficiency and degeneration of the corresponding lumbar discs. This shouldn’t be a surprise because, as Kauppila states, “the disc is located at the end of the nutrient chain, making it one of the first structures to suffer during insufficient nutrient supply.”
In epidemiological studies, associations between cardiovascular risk factors and low back pain (or disc degeneration) are weaker and conflicting. Nevertheless, several studies have linked high blood cholesterol and smoking with low back pain and disc degeneration. It’s important to remember that correlation is different from causation and more research is needed to determine a cause and effect relationship. So, a healthy diet and abstinence from smoking may play a role in the prevention and treatment of low back pain. Further still, and this is pure conjecture on my part, they may have a role to play in maintaining the health of all poorly vascularised tissues (spinal discs, tendons, articular cartilage of joints, etc.).
Yoga Beneficial For Longstanding Low Back Pain
- At August 9, 2017
- By Healing In Motion
- In Research
 0
0
![]()
Last month Groessl et al., from the San Diego School of Medicine, published the results of their study examining the benefits of yoga on military veterans with chronic low back pain. Of the 150 participants in the study, 35% were unemployed or disabled and the mean back pain duration was 15 years. The mean age was 53 years. The group was generally thought to have “fewer resources, worse health, and more challenges attending yoga sessions than community samples studied previously”.
Hatha yoga classes, designed specifically for people with low back pain, were held twice a week for 12 weeks. They were led by an experienced certified instructor. Home practice (15-20 mins/day) was encouraged. The classes consisted of yoga postures, movement sequences, breathing exercises and brief meditation.
The veterans that completed the study had less disability and less pain. Although the decreases in pain were small, they happened in spite of reduced opioid use.
Paracetamol Ineffective For Back Pain And Osteoarthritis
- At April 6, 2015
- By Healing In Motion
- In Research
 0
0
Most of us have us have used paracetamol at some point in our lives, whether to bring down a fever, for a headache, joint pain or some other painful condition. In fact, if we have a look in our medicine cabinets we’ll probably find a box…or two! Machado et al. from George Institute for Global Health at the University of Sydney recently reviewed the scientific literature with the aim of investigating the efficacy and safety of paracetamol (acetaminophen) in the management of spinal pain and osteoarthritis of the hip or knee. They included 13 randomised controlled trials in their review and the results were published in the BMJ.
They found that for low back pain, paracetamol was ineffective at reducing pain or disability and at improving quality of life. It’s important to point out that by “ineffective”, they mean that paracetamol did not provide more benefit than a placebo. For hip and knee osteoarthritis they found that there was a significant, although not clinically important, effect on pain and disability in the short term. Adverse events were not more likely with paracetamol than placebo but patients taking paracetamol are 4 times more likely to have abnormal results on liver function tests.
Although the clinical importance of the last finding is uncertain, paracetamol has been linked to increasing incidence of mortality, increased risk of cardiovascular, gastrointestinal and renal disease. This study has prompted the BMJ to release an editorial discussing the use of paracetamol for back pain and osteoarthritis. One of the problems for GPs is that the National Institute for Clinical Excellence (NICE) recommends paracetamol as the first port of call for low back pain and arthritis. Taking this option away leaves NSAIDS and opioids which both present even more health risks… Non-pharmalogical options should be pursued and developed i.e. physical activity and exercise, weight loss, nutritional supplements and physiotherapy of course!
What Triggers Low Back Pain?
- At February 9, 2015
- By Healing In Motion
- In Research
 0
0
A study published this month in Arthritis Care and Research by Daniel Steffens et al. from the University of Sydney has looked at the risk factors that could lead to acute low back pain. Acute low back pain is back pain that comes on suddenly and resolves after a few days or weeks as opposed to chronic low back pain which is long-standing.
They surveyed close to 1000 people and asked them about the presence of 12 physical and psychosocial factors up to 4 days before the onset of back pain. The results revealed that a number of triggers were linked to acute low back pain:
- moderate to vigorous physical activity increased the risk by 3
- manual tasks involving awkward postures increased the risk by 8
- being distracted during an activity increased the risk by 25
- age decreased the effect of exposure to heavy loads
- risk was highest between 7 am and mid-day
Over the years, I’ve noticed that the parents of young children have an increased incidence of low back pain. Having seen some of the risk factors high-lighted in this study, it becomes evident how sleep-deprived, fatigued and distracted parents that often lift their children in awkward positions can dramatically increase the risk of low back pain. It’s also interesting to note that distraction seems to massively increase the risk of low back pain and therefore underlines the importance of mindfulness.
MBT: To Wear Or Not To Wear?
- At September 21, 2013
- By Healing In Motion
- In Research
 0
0
Ever wondered whether MBT shoes really work? Well, a study was commissioned by companies that manufacture rocker sole shoes. The research was carried out by a team of physiotherapists from King’s College London. 115 people with chronic low back pain (CLBP) were randomly split into 2 groups; one was asked to wear rocker shoes for a minimum of 2 hours a day and the other was asked to wear flat soled shoes for the same duration. The subjects were followed for a year. At the end of the study the researchers concluded that “rocker sole shoes appear to be no more beneficial than flat sole shoes in affecting disability and pain outcomes in people with CLBP. Flat shoes are more beneficial for LBP aggravated by standing or walking.”
Can Antibiotics Cure Low Back Pain?
- At May 13, 2013
- By Healing In Motion
- In News
 0
0
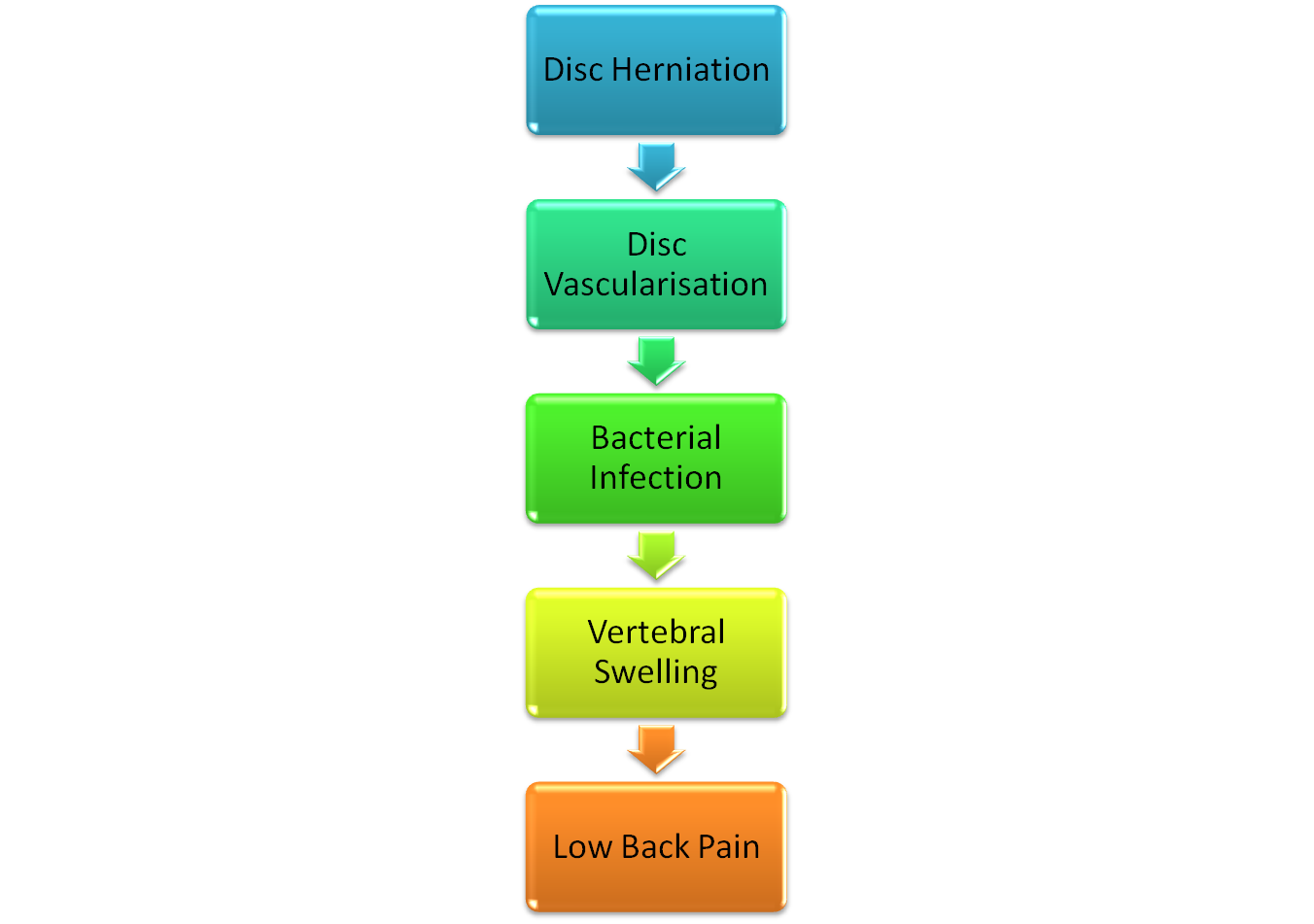
![]() Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
Last week I picked up a copy of Metro and came across an article entitled “Back pain ‘cured with a £114 dose of antibiotics'”. The story has also been covered by theguardian, The Times and the NHS. It’s based on the results of 2 studies published in the European Spine Journal by Hanne B Albert et al. from the University of Southern Denmark. It appears that oedema (swelling) of the vertebrae is observed in 6% of the general population and in 35-40% of people with low back pain. In their first study, Albert et al. examined 61 patients that had MRI-confirmed disc herniation and were undergoing surgery to address this. The disc material was analysed and it turned out that anaerobic bacteria were present in 43% of patients. Of those with anaerobic bacterial infections, 80% presented with oedema of the vertebrae next to the disc prolapse. Whereas only 44% of patients with negative cultures had bone oedema of adjacent vertebrae. The association between anaerobic bacterial presence and bone swelling was highly statistically significant. It’s thought that bacteria reach the inside of intervertebral discs via newly formed blood vessels that penetrate the damaged discs. The flow chart below shows how the process takes place.
In their second study, Albert et al. conducted a double-blind randomised controlled trial with 162 patients whose only known illness was chronic low back pain of greater than 6 months duration occurring after a previous disc herniation. They also had bone edema in the vertebrae next to the previous herniation. The patients were split into 2 groups. One group was given antibiotics for 100 days and the other group was given a placebo for 100 days. The patients were evaluated at the start of treatment, at the end of treatment and 1 year after the end of treatment. The patients given antibiotics improved on all measures; they had less low back pain, less leg pain and better function and the changes were highly statistically significant.
Although these results are extremely encouraging, they should be confirmed with larger groups. Additionally, it’s worth bearing in mind that this form of treatment only applies to a subgroup of people with low back pain and that the indiscriminate use of antibiotics for low back pain should be discouraged as it could lead to decreased efficacy of antibiotics through the spread of drug-resistant bacteria.